
This is the question that haunts almost every patient who finally finds relief through Vestibular Rehabilitation Therapy (VRT). It is frustrating to realize that you may have spent months or even years cycling through specialists, only to discover that the solution was a specialized form of physical therapy that your primary doctor never mentioned.
Understanding the internal mechanics of the medical system can help you navigate this gap without losing your mind—or your hope.

The Pharmacological Bias of Western Medicine
The most significant hurdle is that Western medicine is fundamentally designed around medical management through pharmacological intervention. In medical school, the vast majority of training hours are dedicated to biochemistry and the use of medications to suppress symptoms.
When a patient reports dizziness, the “standard of care” often defaults to:
Suppression: Prescribing medications like meclizine or benzodiazepines to “quiet” the inner ear ot balance center in the brain.
Imaging: Ordering an MRI or CT scan to rule out a stroke or tumor.
Observation: The “wait and see” approach.
While these tools are excellent for ruling out life-threatening emergencies, they do nothing to coordinate the brain’s healing. Medications often mask the problem, which can actually delay the natural recovery process because the brain cannot learn to compensate while it is being chemically suppressed.
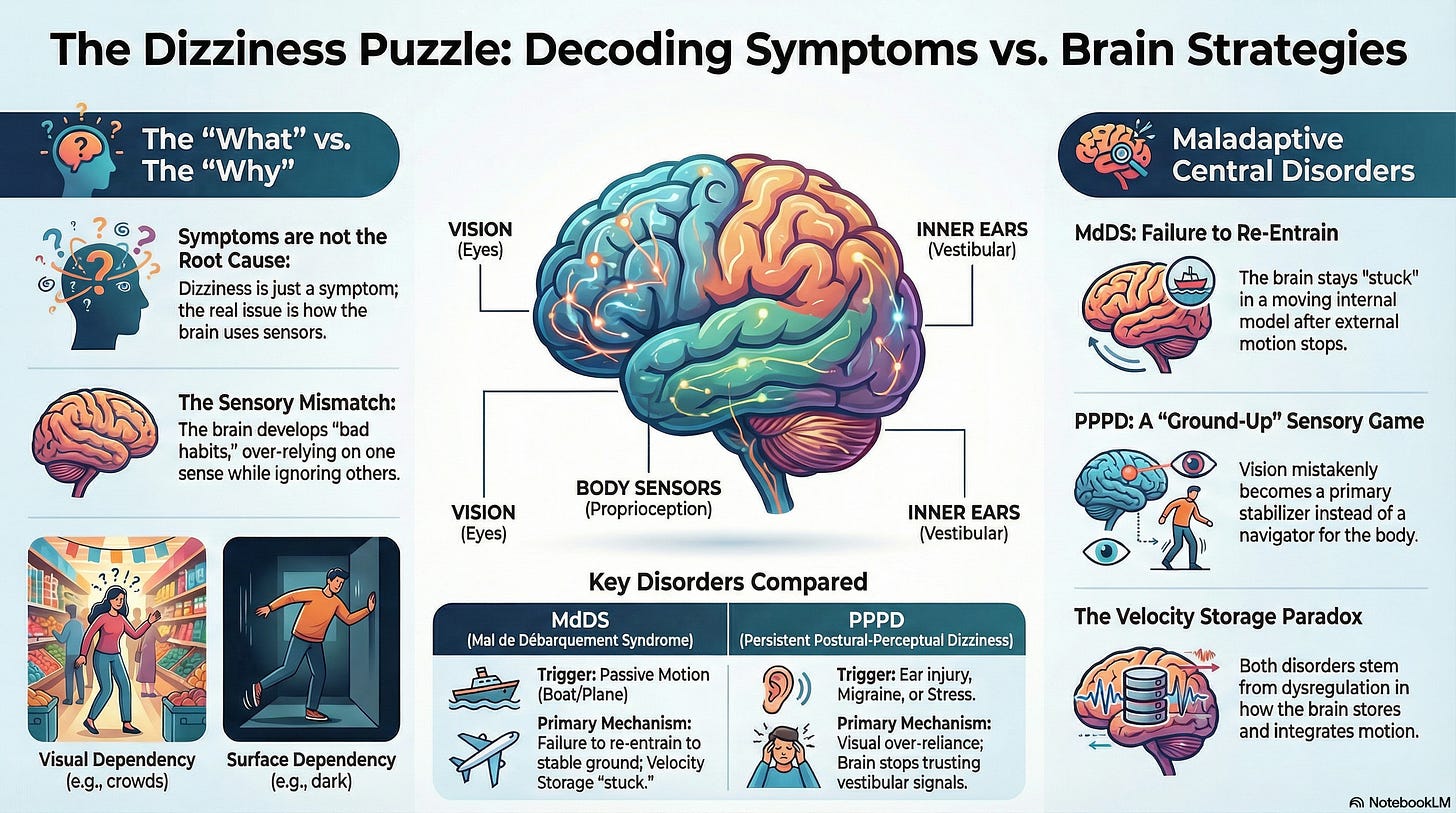
The Complexity of the Word Dizziness
Part of the disconnect stems from the word “dizziness” itself. In the medical world, this is a “garbage pail” term that can mean dozens of different things. Most doctors are not trained to tease out the distinct types of dizziness that dictate a treatment plan.
If you tell a doctor you are “dizzy,” they might hear “lightheaded” (blood pressure), “vertigo” (inner ear), or “unsteadiness” (neurological). Because the terminology is so vague, doctors often feel overwhelmed by the symptom and default to the quickest route: a prescription pad.

A Lack of Functional Training
The Gap in Functional Training
Most physicians receive very little training in the mechanics of how the brain integrates balance. They are trained to find a disease—something they can see on a scan or a blood test. However, vestibular disorders are often functional. The “hardware” (the ear and brain) might look perfect on an MRI, but the “software” (how they talk to each other) is glitching.
Because VRT is a specialized branch of physical therapy, it exists outside the standard medical doctor’s daily toolkit. They may not view VRT as a primary medical intervention simply because it doesn’t involve a pill or a surgery. This lack of functional training means they are looking for something “broken” rather than something that needs to be “recalibrated.”

How to Bridge the Gap Without Resistance
Walking into a doctor’s office and trying to “teach” them neurology can often trigger professional resistance. The goal is to provide them with the functional data they need to justify a specialized referral.
Use Specific Categories: Instead of saying “I’m dizzy,” tell your doctor, “I am experiencing disequilibrium and motion sickness when I move my head.” This helps them move past the “garbage pail” term of dizziness.
Focus on Function: Describe how these symptoms stop you from doing your job, driving, or walking in a grocery store. Doctors are more likely to refer to a specialist when they see a clear functional limitation that medication isn’t fixing.
Be the Expert of Your Symptoms: Once you have a diagnosis, learn everything you can about how your specific environment affects you. When you present clear patterns to your doctor, you are giving them the “why” they need to support a referral.
My Role as a Physical Therapist
As a Physical Therapist specializing in vestibular rehabilitation, my role is to provide the clinical bridge that the standard medical system often misses. I do not just look for “disease”; I look at how your systems coordinate.
I focus on the signaling and the microenvironment of the vestibular system to facilitate a more stable outcome. By identifying which of the five types of dizziness you are experiencing, we can support and optimize your brain’s natural ability to recalibrate. This collaborative approach ensures that your medical team sees VRT not as an “alternative,” but as the essential path to your recovery.


Yes! Doctors ignorance and unwillingness to learn has taken me over 5 years to finally get an up to date accurate dx. Even as recently as Dec 2025 when I saw a Neurologist who was supposed to be familiar with Vestibular issues. He only vaguely heard of PPPD. I was not even asking for a Dx. I was asking for a referral to John Hopkins for a vestibular evaluation. I already knew from all my symptoms that I had PPPD. Maybe he thought he could get me to come back for a few more appointments. He flatly refused to refer me. Finally, I got my primary care doctor. to refer me. I no longer have BBVP thanks to 3 rounds of Physiscal Therapy at 3 different places. I do have PPPD and finally have an official diagnosis. I got a lot of VRT but my balance only got a little better. The BBVP was gone but the PPPD was still there and not diagnosed until recently.
Agree 100%!!!